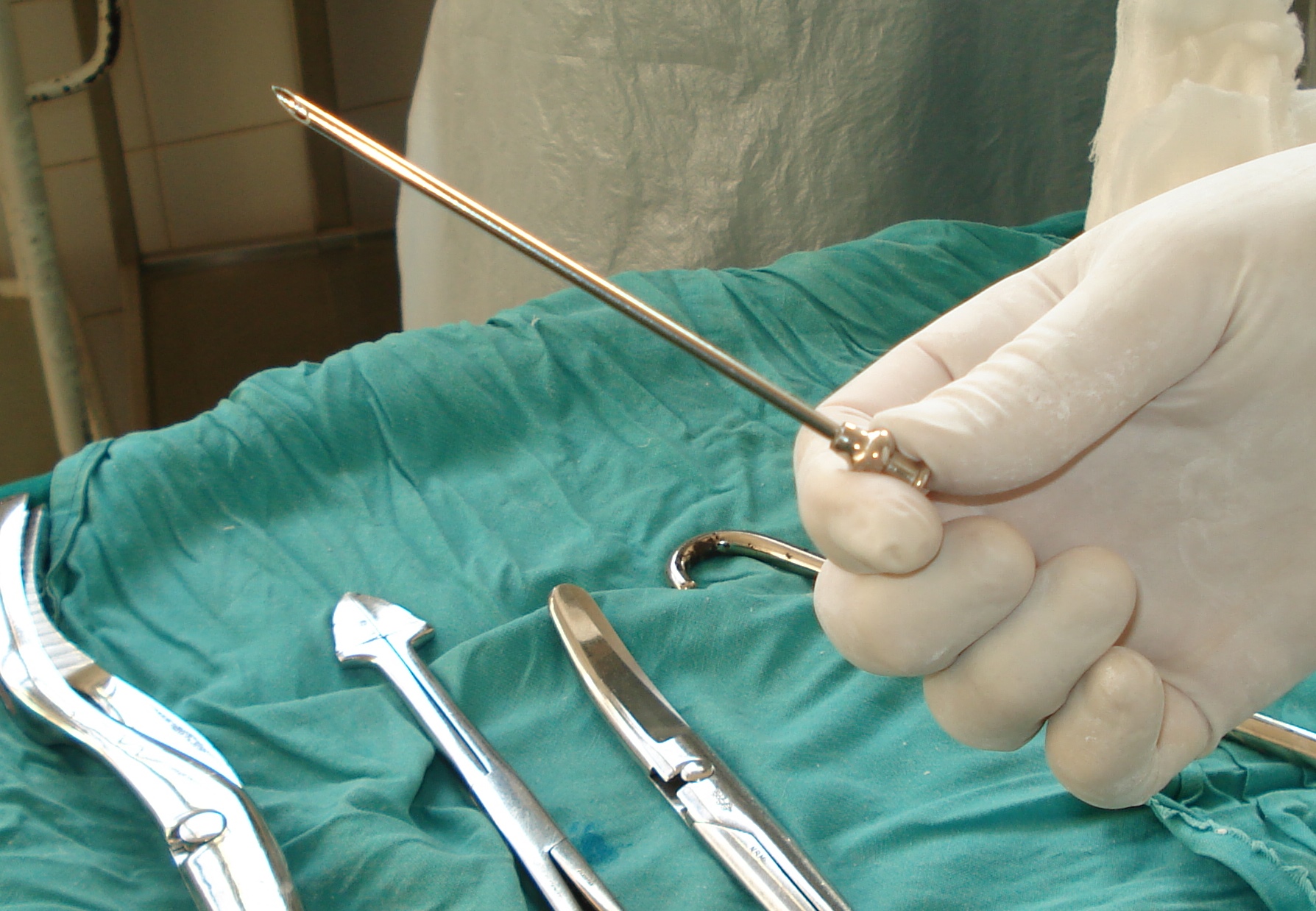
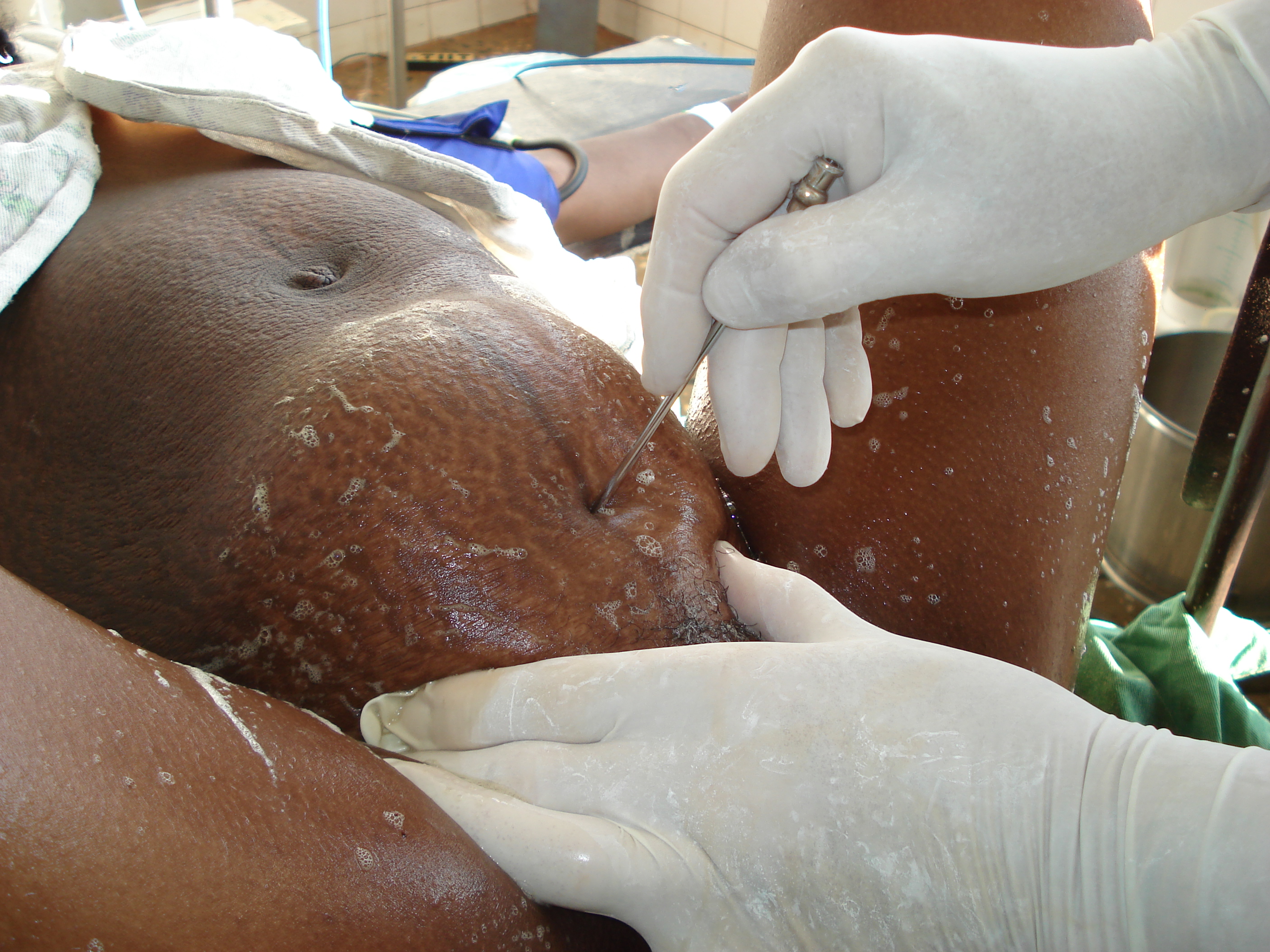
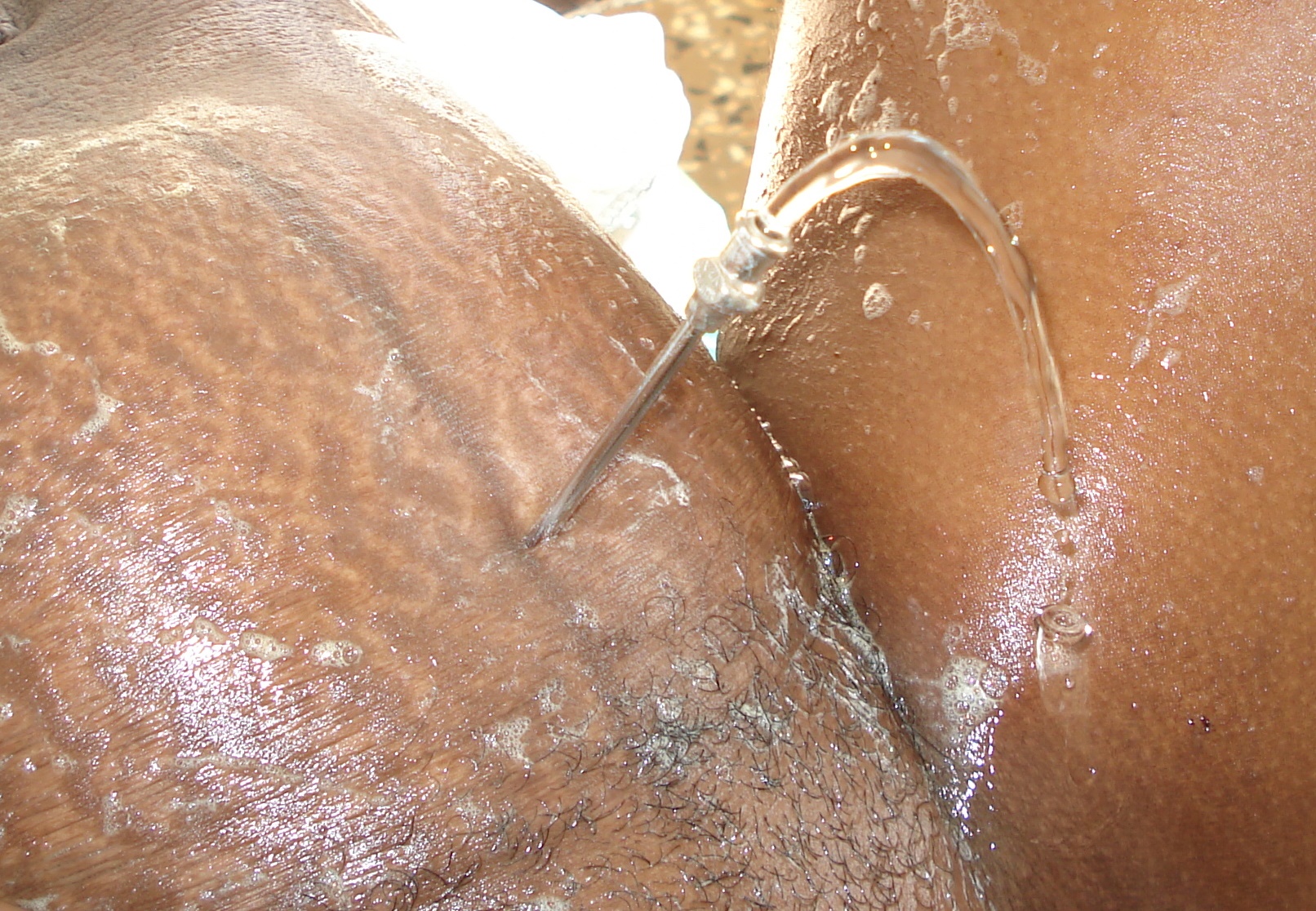
SPINAL
- All obstetrical procedures can be performed in spinal anesthesia
- Preferred method for C/S
- Unless patient is in chock
KETAMINE
- When spinal anesthesia fails
- When spinal anesthesia is contraindicated
- Shock due to
- Sepsis
- Hemorrhage
- Shock due to
- Combine with
- atropine
- valium
- Recommended doses:
PUDENDAL BLOCK / SACRAL ANESTHESIA
- Forceps Delivery
- Episiotomy
LOCAL INFILTRATION ANESTHESIA
- Episiotomy
- Symphysiotomy
- C/S
GENERAL INTUBATION ANESTHESIA
- Uterine Rupture
- C/S in Eclampsia.